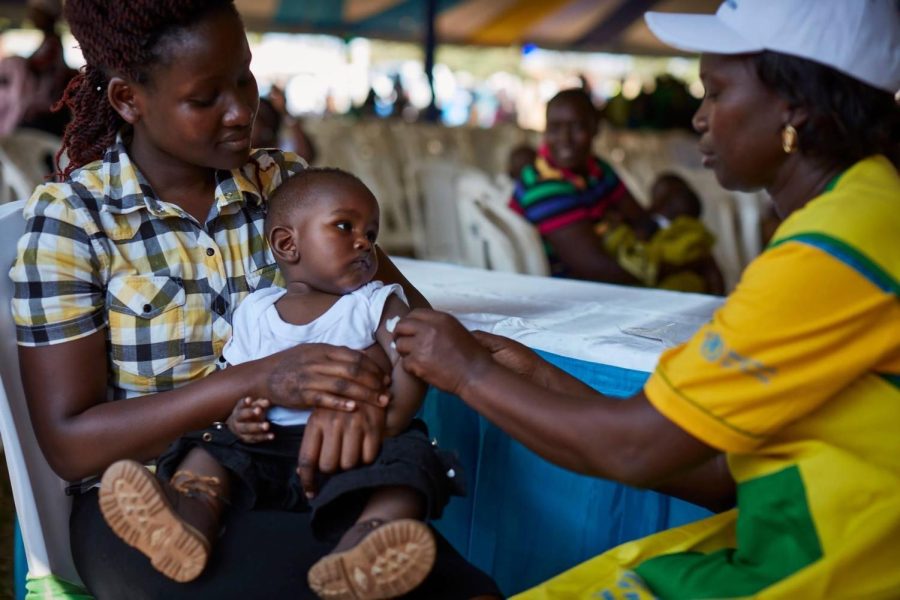
Historical Malaria Vaccine
CDC Foundation capturing a “historic moment in the fight against malaria” as recommendation comes from WHO.
October 29, 2021
On Oct 6th 2021, the World Health Organization (WHO) announced its recommendation of a new Malaria vaccine, Mosquirix (RTS, S/AS01), among children. This is the first malaria vaccine to be approved and many hope it marks a major change. WHO Director-General Dr. Tedros Adhanom Ghebreyesus, described the vaccine as, “a historic moment” and a “breakthrough for science, child health and Malaria control.” The vaccine announcement comes after years of research and attempts to eradicate the disease.
The Center for Communicable Diseases, now known as the Center for Disease Control (CDC) describes Malaria as a parasitic and fatal disease, which tends to infect certain mosquitoes that feed on humans. About 2,000 cases are diagnosed in the U.S. each year. Most of these cases originate from travelers returning from high transmission regions. High rates of Malaria tend to occur in poorer regions, exacerbating issues due to a lack of physical and social infrastructure. Malaria has been eliminated from many developed countries, including the U.S., but continues to have a massive presence in developing countries. In 2019, WHO estimated that 409,000 people died from Malaria, most of which were African children. Discovering treatments and prevention options have been important in increasing the average expected age of death, decreasing infant mortality rates and improving quality of life, all of which correlate with economic development.
Malaria is one of the oldest diseases, even described by Hippocrates. Early antimalarials were developed from the Cinchona tree, also known as chloroquine. During WWII, Cinchona became inaccessible, so research for more quinine treatments expanded. Outbreaks in the 20th century resulted in the development of the CDC, dedicated to the eradication of Malaria in the U.S. Later, after its elimination in 1951, the CDC refocused its efforts. In working with the WHO, a global campaign to eliminate Malaria was launched in 1955. There were some positive impacts of the campaign, but ultimately the complexity of the disease made elimination extremely difficult. Notably, the sub-Saharan region was excluded from the program entirely.
The Mosquirix vaccine is impactful because of its effectiveness in children. The WHO recommendation came after considering 2 years of research from child health clinics in Ghana, Kenya, and Malawi. Sub-saharan Africa continues to be the most impacted by Malaria. When discussing what this vaccine and recommendation means, WHO Regional Director for Africa, Dr. Matshidiso Moeti, said it “offers a glimmer of hope for the continent which shoulders the heaviest burden of the disease.” The implications of the vaccine’s feasibility means a more equitable distribution among the already disadvantaged.
There are concerns as to where the resources for administering these vaccines will be found. Furthermore, to be fully vaccinated, a child must have 4 injections over 2 years. Still, many healthcare professionals, especially those working around malaria, hope it furthers aid in eliminating this preventable disease.